Australian doctors have reported a surge in the number of people cancelling their vaccine appointments, amid a new wave of caution over the AstraZeneca jab.
It comes after the government updated guidance last week to recommend only those aged over 60 get the shot, due to the risk of a rare blood-clotting syndrome.
Under-60s have been advised to get the alternative Pfizer shot, of which there are limited supplies.
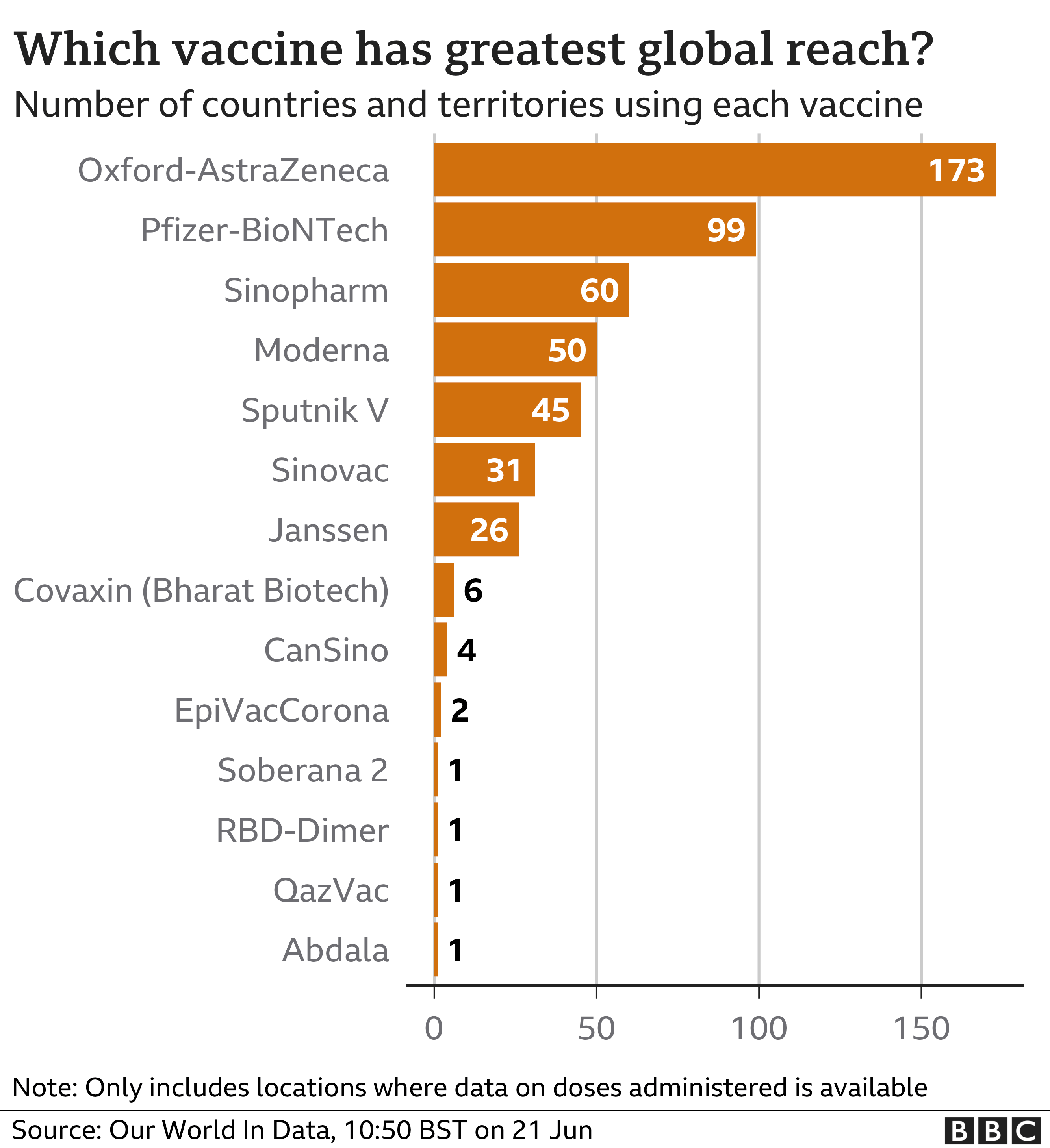
Turning down any vaccine – and AstraZeneca is the world’s most widely used one – may seem remarkable to other nations still battling rampant Covid.
But Australia is one of the few nations where the virus has never truly taken hold. So for many locals, even amid new outbreaks in Sydney and Melbourne, the risk of catching Covid is seen as lower than developing a rare blood clot.
Vaccine hesitancy has been an issue in Australia for months. But experts now fear the government’s latest downgrade has hindered the nation’s vaccination progress.
“All across the country people are cancelling appointments or asking about whether they should even have their second dose,” says Dr Karen Price, president of the Royal Australian College of General Practitioners.
“It has definitely put a big barrier on the vaccine rollout,” she told the BBC.
“We’re going to have to regroup and regain confidence in it, as it’s really important to keep the vaccination programme rolling out. We still have elderly people unvaccinated, and we’re seeing community transmission again.”
What has Australia said about AstraZeneca’s vaccine?
Australia’s vaccine programme began in February, and is currently open to all aged over 40.
But so far only 3% of adults have been vaccinated, while nearly 25% have received a first shot.
Comparatively, it is far behind many other Western nations, partly due to citizens’ vaccine hesitancy, but also due to the government’s missteps in securing supplies.
Until April, the government had relied upon AstraZeneca to be its main jab vaccinating the nation. Local labs were set up to churn out its production.
But when reports emerged of the thrombosis and thrombocytopenia syndrome, a rare blood clotting occurrence linked to the vaccine, the government advised people under 50 to take a different vaccine.
The catch was that Australia only had one other vaccine – the Pfizer shot – in significantly smaller quantities. The government has promised there will be enough supplies of Pfizer or other vaccines, like Moderna and Novovax, by the final quarter of the year.
But the decision by Australia’s vaccine safety body last week to limit AstraZeneca’s use even further, to those aged 50 to 59, pushed another two million people into the Pfizer-reliant group.
It also raised concerns among Australians left with AstraZeneca as their only vaccine option.
What is AstraZeneca’s risk, and why are Australians fearful?
Australia changed its advice last week because it found more clotting cases among those in their 50s – a risk of 2.7 clotting cases per 100,000 first doses.
The risk is 3.1 cases per 100,000 doses for those under 50.
But experts say that such a risk is still extremely low, and the decision to limit the vaccine is done in the context of Australia’s low Covid cases.
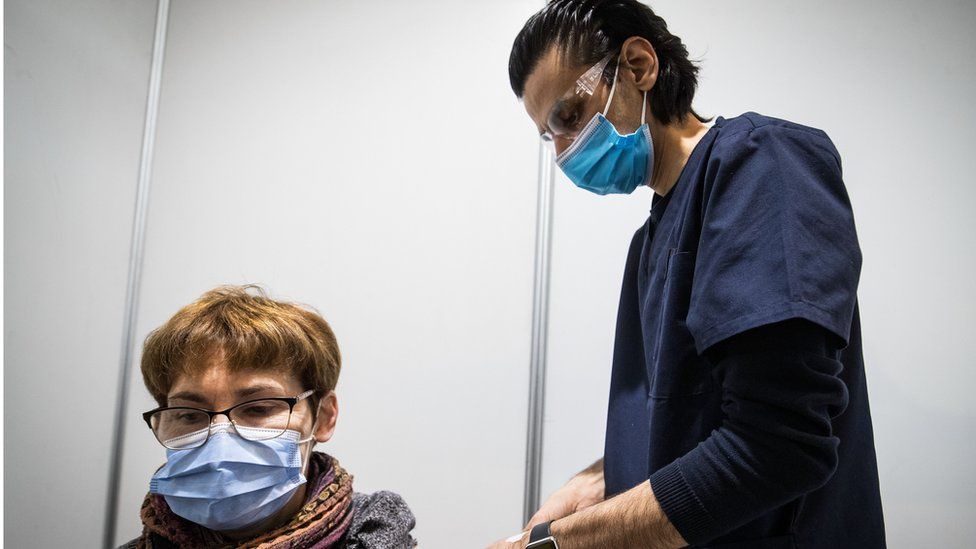
Authorities are urging patients who’ve gotten their first jab to stay the course and get their second dose, noting the clotting risk is even 10 to 15 times lower. Data from the UK’s AstraZeneca rollout showed just 1.5 clotting cases per million second doses.
But GPs, who are administering the vaccine at clinics and facing patients’ questions, say statistics aren’t enough to assuage fears.
People want the Pfizer vaccine instead, says Dr Todd Cameron, a Melbourne GP who runs several clinics in the city. He has had hundreds of AstraZeneca bookings cancelled, despite the city recently emerging from lockdown due to a new case outbreak.
“The problem is that there’s a public perception that there are two vaccines – the good one and the less good one and so people are reasonably saying, ‘Well why can’t I have the good one?’
“They’re also saying ‘Why am I in the group that doesn’t have access?'”
The risk in getting AstraZeneca has been often compared to other risks, such as complications with the pill for women, or the chance of dying from a lightning strike or in a car crash. Statistically, those are all higher.
But Dr Cameron says patients end up comparing the AstraZeneca risk to that of Pfizer – the other vaccine option.
What could help in getting Australians vaccinated?
Australia still heavily relies on the AstraZeneca jab for its vaccination programme.
It has pledged to get a first dose of any vaccine available to everyone by the end of the year.
But given this latest hit to AstraZeneca’s image, experts say it’s crucial now that the government rolls out better public health messaging to achieve its goals.
“What we really need is an easy-to-understand national advert campaign, where the message doesn’t necessarily come from authorities but people that other people can relate to,” says Dr Price.
GPs across the country have vented frustrations about the burden of having to be the main communicators about the vaccine. Typically, patients are still lobbing their first questions about AstraZeneca to GPs instead of going into clinics already informed, they say.
“We feel like we’re having to be a little apologist for government policy, having to explain something where in the vast majority of cases people want something else,” says Dr Cameron.
“There’s been a complete absence of effective public health messaging about the vaccine.”
The government has said an advertising campaign is in the works, but will not be rolled out until vaccine supply has been confirmed.